Chapter 13 Poor Response to TCS - Contact Dermatitis?
I guess there are no dermatologists who do not know of Fisher’s Contact Dermatitis, which provides an essential database to check for patch test concentration of suspected substances. I also consulted it many times.
Chapter 15 of the sixth edition published in 2008 covers topical corticosteroids (TCS).
This chapter outlines contact dermatitis (rash) caused by TCS. Topical corticosteroids are the drugs for suppressing a rash, but some people develop an allergic reaction and aggravate a disease flare by applying them. We can confirm this with patch testing.
The following is the excerpt from the outset.
----- Excerpt -----
Reactions to topical corticosteroids or their vehicles should be suspected when the use of the topical corticosteroids either does not improve the existing dermatitis or makes it worse. One should be alerted particularly when a patient has used a topical corticosteroid with a good response but then no longer responds, or the existing dermatitis becomes worse. If a patient with a corticosteroid-responsive dermatosis does not respond appropriately, one could consider the possibility that corticosteroid allergy might be the reason for a lack of response. In a study of 41 such cases, 9 or 22% were found to be allergic to corticosteroids.
----- End of excerpt -----
This is a textbook for contact dermatitis and it stresses the possibility of contact dermatitis caused by TCS in light of the study reporting a positive patch test reaction in 22% of 41 patients.
The above fact also reveals that TCS got less effective or worsened the dermatitis in 32 patients (78%) although they were not allergic to TCS.
I read the reference material (the study of 41 cases) out of interest.
Detection of contact hypersensitivity to corticosteroids in allergic contact dermatitis patients who do not respond to topical corticosteroids
Published in the Contact dermatitis Volume 53 Issue 2 , Pages 67 - 123 (August 2005)
A dermatologist in Turkey wrote this paper. The original disease of patients is only mentioned as allergic contact dermatitis. This might be dermatitis that looked like a rash with causes unknown. Out of 41 patients, 32 had a rash due to some reasons many times, and 8 had stasis dermatitis on the thigh. It seems 24 had eczema on their hands.
According to this paper, 32 patients out of 41 showed positive reactions of some kind or another in a standard series of patch tests. Seven types of steroids were used and 9 (22%) had a positive reaction to at least one of them.
Positive reaction in standard series patch tests does not always define the causes for eczema. Positive reaction against steroids does not always mean the absolute allergen is a steroid. It is only after the inflammation has disappeared by eliminating the contact with suspected substances when the allergens are determined and diagnosis of contact dermatitis can be made. Patch test results are just a clue. On the other hand, if patch test reaction against TCS is negative, an allergen is thought to be TCS if the rash is cleared soon after the stoppage (in that case, there was something wrong with patch testing).
This paper only shows the patch test result for steroids and does not mention how many of these 41 patients recovered. It just estimates that a corticostesteroid allergy is a causative reason for a poor reaction to TCS in 9 out of 41 patients.
I have seen many patients with hand eczema or thigh stasis dermatitis, which fall into steroid addiction and take the course of TCS discontinuation, then rebound to remission. It is possible that patients get addicted even though their primary disease is not atopic dermatitis. It might be because TCS tends to be used for a long time.
Below is the excerpt from the book I wrote, Color Atlas of Steroid Withdrawal from Topical Corticosteroid in Patients with Atopic Dermatitis, published by Ishiyaku Publishers in 2000.
----- Excerpt -----
Steroid skin syndrome in various skin diseases, but not in atopic dermatitis
The cases presented in this chapter are considered to be necessary for understanding the concept of so-called “steroid skin syndrome”, though they may deviate from the outline of this book, that is, steroid withdrawal in atopic dermatitis.
Steroid skin syndrome is the condition in which a stronger or more various aggravations of the eruption stemmed from discontinuation of application of steroids after long-term use.
Steroid skin syndrome is different from classic adverse effects such as rosacea, acne or skin atrophy caused during application of the steroid ointment. It is difficult to notice for doctors because there is no symptom during application of steroids, but symptoms emerge for the first time after discontinuation of them.
Steroid skin syndrome is not limited to atopic dermatitis. Paradoxically, there are cases that secede easily from steroids without any rebound even if large amounts of steroid are applied to skin.
It seems to be true that there is a group of patients who became easily steroid-addicted after continuous application of steroid ointment, and the ratio of such patients is high in patients with atopic dermatitis.
1. Steroid skin syndrome in Hand Eczema
Though this type of steroid skin syndrome is not a matter of great importance at present, the author thinks that a considerable amount of potential cases are occurring. It often happens that serum IgE values are found high and RAST scores are positive through blood tests for studying an atopic predisposition because the rebound phenomena were observed after steroid discontinuation.
I guess there are no dermatologists who do not know of Fisher’s Contact Dermatitis, which provides an essential database to check for patch test concentration of suspected substances. I also consulted it many times.
Chapter 15 of the sixth edition published in 2008 covers topical corticosteroids (TCS).
This chapter outlines contact dermatitis (rash) caused by TCS. Topical corticosteroids are the drugs for suppressing a rash, but some people develop an allergic reaction and aggravate a disease flare by applying them. We can confirm this with patch testing.
The following is the excerpt from the outset.
----- Excerpt -----
Reactions to topical corticosteroids or their vehicles should be suspected when the use of the topical corticosteroids either does not improve the existing dermatitis or makes it worse. One should be alerted particularly when a patient has used a topical corticosteroid with a good response but then no longer responds, or the existing dermatitis becomes worse. If a patient with a corticosteroid-responsive dermatosis does not respond appropriately, one could consider the possibility that corticosteroid allergy might be the reason for a lack of response. In a study of 41 such cases, 9 or 22% were found to be allergic to corticosteroids.
----- End of excerpt -----
This is a textbook for contact dermatitis and it stresses the possibility of contact dermatitis caused by TCS in light of the study reporting a positive patch test reaction in 22% of 41 patients.
The above fact also reveals that TCS got less effective or worsened the dermatitis in 32 patients (78%) although they were not allergic to TCS.
I read the reference material (the study of 41 cases) out of interest.
Detection of contact hypersensitivity to corticosteroids in allergic contact dermatitis patients who do not respond to topical corticosteroids
Published in the Contact dermatitis Volume 53 Issue 2 , Pages 67 - 123 (August 2005)
A dermatologist in Turkey wrote this paper. The original disease of patients is only mentioned as allergic contact dermatitis. This might be dermatitis that looked like a rash with causes unknown. Out of 41 patients, 32 had a rash due to some reasons many times, and 8 had stasis dermatitis on the thigh. It seems 24 had eczema on their hands.
According to this paper, 32 patients out of 41 showed positive reactions of some kind or another in a standard series of patch tests. Seven types of steroids were used and 9 (22%) had a positive reaction to at least one of them.
Positive reaction in standard series patch tests does not always define the causes for eczema. Positive reaction against steroids does not always mean the absolute allergen is a steroid. It is only after the inflammation has disappeared by eliminating the contact with suspected substances when the allergens are determined and diagnosis of contact dermatitis can be made. Patch test results are just a clue. On the other hand, if patch test reaction against TCS is negative, an allergen is thought to be TCS if the rash is cleared soon after the stoppage (in that case, there was something wrong with patch testing).
This paper only shows the patch test result for steroids and does not mention how many of these 41 patients recovered. It just estimates that a corticostesteroid allergy is a causative reason for a poor reaction to TCS in 9 out of 41 patients.
I have seen many patients with hand eczema or thigh stasis dermatitis, which fall into steroid addiction and take the course of TCS discontinuation, then rebound to remission. It is possible that patients get addicted even though their primary disease is not atopic dermatitis. It might be because TCS tends to be used for a long time.
Below is the excerpt from the book I wrote, Color Atlas of Steroid Withdrawal from Topical Corticosteroid in Patients with Atopic Dermatitis, published by Ishiyaku Publishers in 2000.
----- Excerpt -----
Steroid skin syndrome in various skin diseases, but not in atopic dermatitis
The cases presented in this chapter are considered to be necessary for understanding the concept of so-called “steroid skin syndrome”, though they may deviate from the outline of this book, that is, steroid withdrawal in atopic dermatitis.
Steroid skin syndrome is the condition in which a stronger or more various aggravations of the eruption stemmed from discontinuation of application of steroids after long-term use.
Steroid skin syndrome is different from classic adverse effects such as rosacea, acne or skin atrophy caused during application of the steroid ointment. It is difficult to notice for doctors because there is no symptom during application of steroids, but symptoms emerge for the first time after discontinuation of them.
Steroid skin syndrome is not limited to atopic dermatitis. Paradoxically, there are cases that secede easily from steroids without any rebound even if large amounts of steroid are applied to skin.
It seems to be true that there is a group of patients who became easily steroid-addicted after continuous application of steroid ointment, and the ratio of such patients is high in patients with atopic dermatitis.
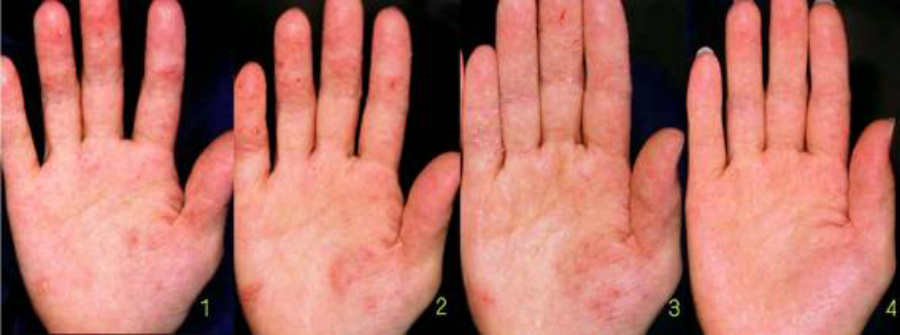
1. Steroid skin syndrome in Hand Eczema
Though this type of steroid skin syndrome is not a matter of great importance at present, the author thinks that a considerable amount of potential cases are occurring. It often happens that serum IgE values are found high and RAST scores are positive through blood tests for studying an atopic predisposition because the rebound phenomena were observed after steroid discontinuation.
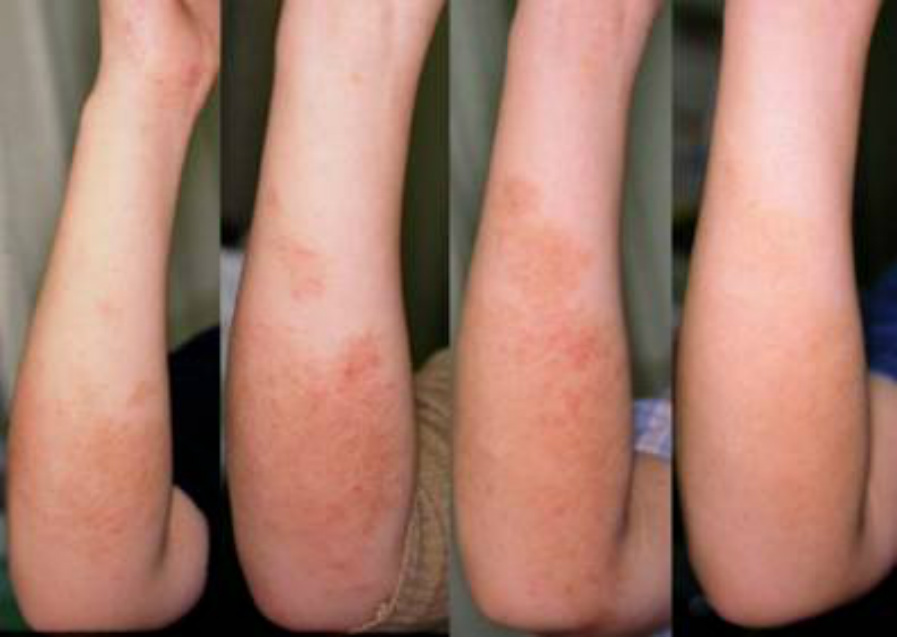
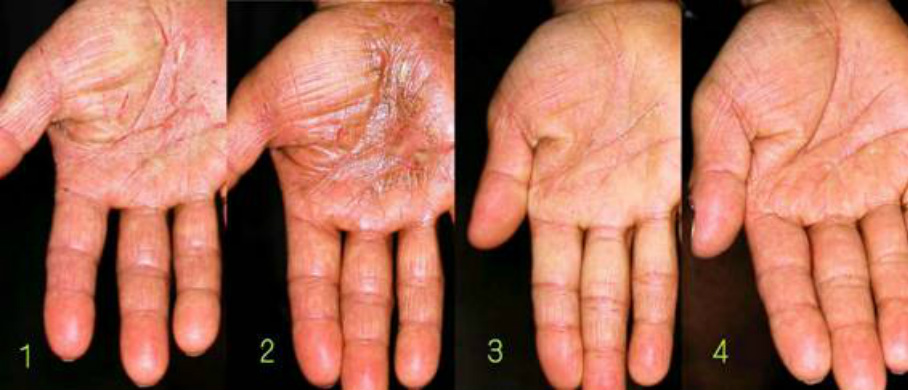
The rebound eruption is limited only on hands in some cases, but it disappears after causing eczema in the arm or the elbow when the hand lesion is improved, like in this case. There are cases in which continuous steroid-resistant eczema is limited to one finger at first, but it expands to the arm and trunk after steroid discontinuation and then it causes erythroderma. The rebound phenomenon also occurs in parts of the body to which the steroids have never been applied.
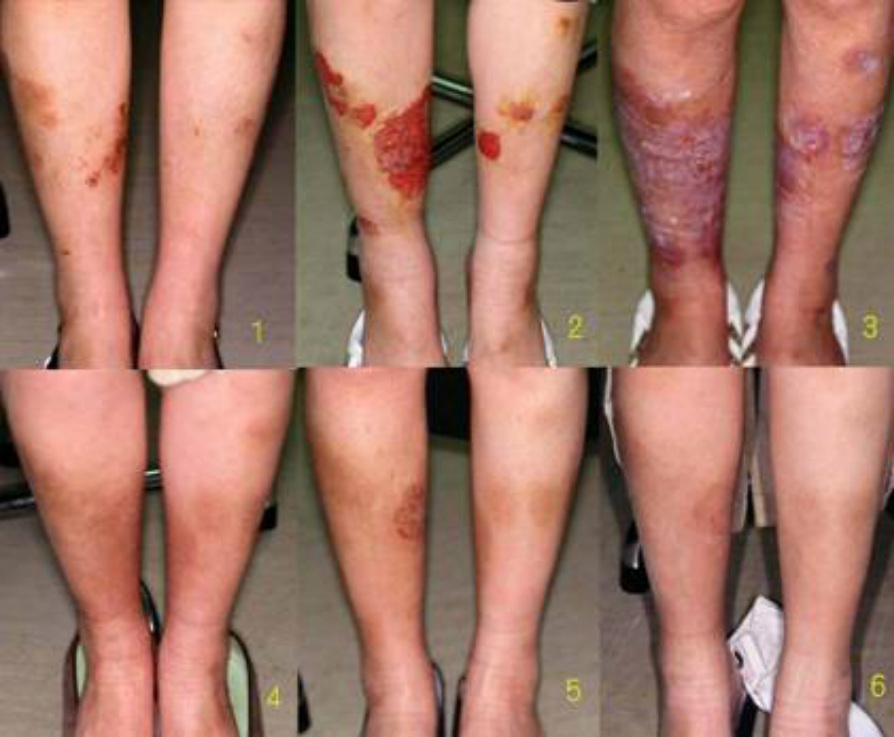
2. Steroid skin syndrome in Nummular Eczema
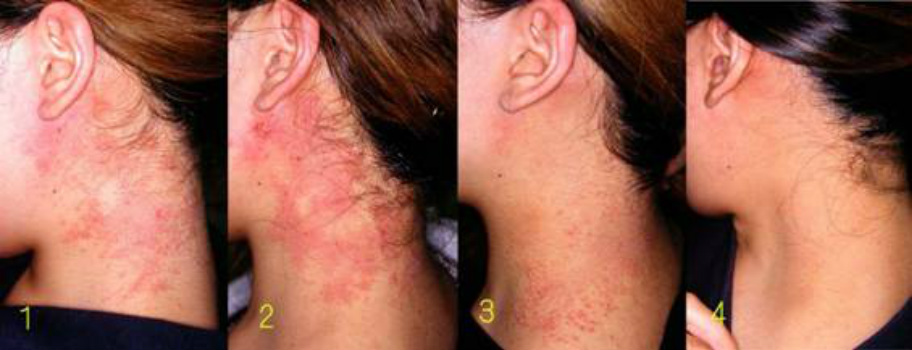
Intractable nummular eczema, which expands after steroid cessation and resides gradually.
Resembling Type 3 (geographically diffusing pattern) and hand eczema case, clinical presentation is nummular eczema itself.
Intractable nummular eczema, which expands after steroid cessation and resides gradually.
Resembling Type 3 (geographically diffusing pattern) and hand eczema case, clinical presentation is nummular eczema itself.
(After steroid cessation, rebound flare developed (pictures 2 and 3) and then resided. It recurred a little (5), but healed (6) by applying white petrolatum without using steroids.
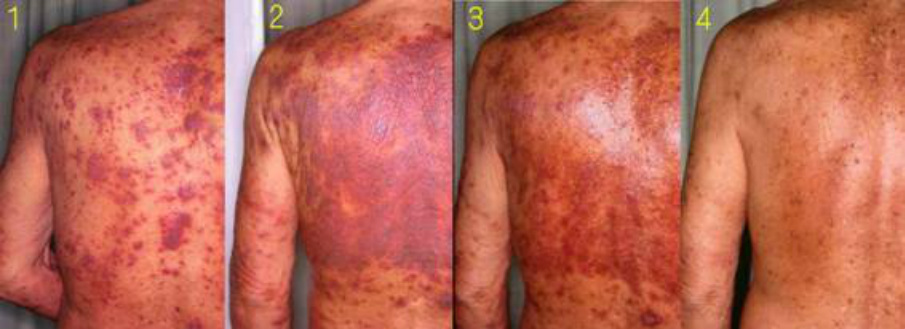
3. Steroid skin syndrome with Senile Xerosis
Judging from the process, initial senile xerosis changed into steroid dermopathy through long term use of topical corticosteroids.
This case is considered potentially to occur often in number and can be a problem in the future.
3. Steroid skin syndrome with Senile Xerosis
Judging from the process, initial senile xerosis changed into steroid dermopathy through long term use of topical corticosteroids.
This case is considered potentially to occur often in number and can be a problem in the future.
4. Steroid skin syndrome with Palmo-Planter Pusturosis
It looks like pustulosis palmaris et plantaris, but is actually steroid dermopathy. It will be cured going through withdrawal and rebound.
It looks like pustulosis palmaris et plantaris, but is actually steroid dermopathy. It will be cured going through withdrawal and rebound.
5. Steroid skin syndrome resembling Contact Dermatitis
A rush is limited in area and suspected to be contact dermatitis. But it is steroid dermopathy in reality and will be cured going through withdrawal and rebound.
A rush is limited in area and suspected to be contact dermatitis. But it is steroid dermopathy in reality and will be cured going through withdrawal and rebound.
----- End of excerpt -----
I suspect that steroid addicted patients are included in the 41 cases reported by the Turkish dermatologist.
Let’s get back to the book by Fisher. The below is continued from the excerpt indicated at the outset of this chapter (Chapter 15 of Fisher’s Contact Dermatitis).
----- Excerpt -----
Children with atopic dermatitis are exposed to topical corticosteroids over prolonged periods of time. A study of 71 children with atopic dermatitis and use of topical corticosteroids for greater than 6 months in the prior 2 years found that 18 (25.3%) reported aggravation or lack of improvement in the dermatitis with such treatment. While this might suggest a corticosteroid allergy, only one child proved to be sensitive in patch testing.
----- End of excerpt -----
I also read the following reference material.
Contact allergy to topical corticosteroids in children with atopic dermatitis
Published in the Contact Dermatitis 2005: 52: 162–163
This is the report by an Italian dermatologist. Discussion includes the following description: “In our study, the contact sensitization to topical corticosteroids resulted rare in AD children, despite the prolonged use of topical corticosteroids. This might be explained by downregulation of the Th1 cells in AD subjects.”“ Corticosteroid contact allergy does not seem to explain a significant number of patients with aggravation of AD during topical corticosteroid treatment.”
There is no reference to addiction, but I predict steroid addictive patients are included in the 18 cases cited above.
It is natural that Fisher should suggest patch testing, in Chapter 15 of Contact Dermatitis, suspecting the steroid itself is a cause for contact dermatitis when he found many chronic skin disorder cases where topical corticosteroids did not work or worsened the inflammation because it is a textbook of the contact dermatitis.
I think that lower-than-expected rate of positive patch test reaction against steroids implies the existence of many steroid addicted cases in patients with atopic dermatitis.
I suspect that steroid addicted patients are included in the 41 cases reported by the Turkish dermatologist.
Let’s get back to the book by Fisher. The below is continued from the excerpt indicated at the outset of this chapter (Chapter 15 of Fisher’s Contact Dermatitis).
----- Excerpt -----
Children with atopic dermatitis are exposed to topical corticosteroids over prolonged periods of time. A study of 71 children with atopic dermatitis and use of topical corticosteroids for greater than 6 months in the prior 2 years found that 18 (25.3%) reported aggravation or lack of improvement in the dermatitis with such treatment. While this might suggest a corticosteroid allergy, only one child proved to be sensitive in patch testing.
----- End of excerpt -----
I also read the following reference material.
Contact allergy to topical corticosteroids in children with atopic dermatitis
Published in the Contact Dermatitis 2005: 52: 162–163
This is the report by an Italian dermatologist. Discussion includes the following description: “In our study, the contact sensitization to topical corticosteroids resulted rare in AD children, despite the prolonged use of topical corticosteroids. This might be explained by downregulation of the Th1 cells in AD subjects.”“ Corticosteroid contact allergy does not seem to explain a significant number of patients with aggravation of AD during topical corticosteroid treatment.”
There is no reference to addiction, but I predict steroid addictive patients are included in the 18 cases cited above.
It is natural that Fisher should suggest patch testing, in Chapter 15 of Contact Dermatitis, suspecting the steroid itself is a cause for contact dermatitis when he found many chronic skin disorder cases where topical corticosteroids did not work or worsened the inflammation because it is a textbook of the contact dermatitis.
I think that lower-than-expected rate of positive patch test reaction against steroids implies the existence of many steroid addicted cases in patients with atopic dermatitis.