Chapter 12 Classification of Eruption during Withdrawal Process
As I mentioned in the previous chapter, it is usually impossible (not always) to diagnose addiction or rebound phase with a single picture taken at one occasion. But we notice several patterns of development by sorting through time-series pictures for many cases.
I once published these paternal cases as the atlas for steroid withdrawal care (Color Atlas of Steroid Withdrawal from Topical Corticosteroid in Patients with Atopic Dermatitis, Ishiyaku Publishers, 2000). Below is the excerpt from this book.
----- Excerpt -----
Preface
I bet it is not easy to stop administering topical corticosteroids (TCS) to patients with atopic dermatitis (AD) for dermatologists who have not taken such measures.
This book visually describes the process of AD patients withdrawing from steroid addiction through recurrence of severe flare (rebound) with time-series color pictures.
There are some patterns in recurrence of AD flare (rebound flare) accompanying TCS withdrawal and the remission processes are classified into several types. This book was written to pass such information to dermatologists with littlie experience in the topical steroid withdrawal.
AD can be treated effectively with TCS for a short duration. But long time application is likely to cause severe recurrence of AD flare (rebound) after cessation.
I’d be happy if this book provides useful materials for dermatologists in objectively reviewing how to utilize TCS for AD treatment from the specialist’s viewpoint.
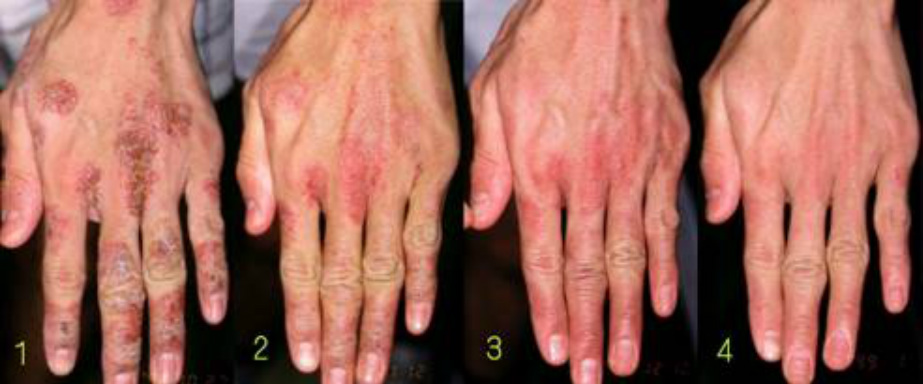
Type 1 Flush and plaque pattern
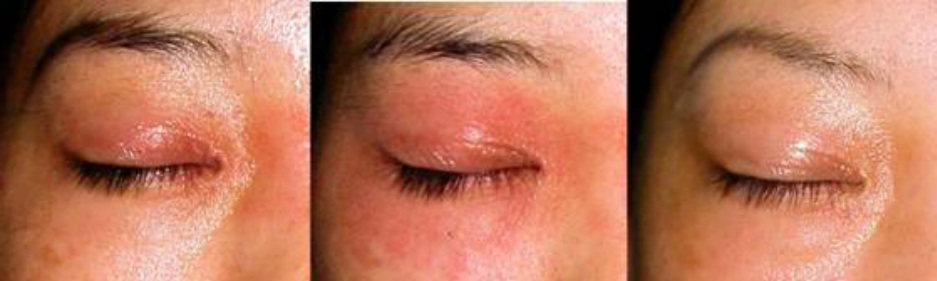
The lesion is characterized by poorly demarcated flushed plaques. In some severe cases, an entire body is flushed or erythroderma develops, but the cutaneous findings are simple and rarely present pigmentation, prurigo or lichenification.
When erythroderma develops, clearly demarcated flushed plaque frequently appears on the wrists or ankles.
This type is regarded as nearly pure atopic dermatitis because it is observed also in patients with no use of steroids for a long time after withdrawal and babies or infants with little use of steroids.
The flushed plaque may progress to exudative erythematous appearance in prolonged cases in which rebounds persist for months or over one year.
As I mentioned in the previous chapter, it is usually impossible (not always) to diagnose addiction or rebound phase with a single picture taken at one occasion. But we notice several patterns of development by sorting through time-series pictures for many cases.
I once published these paternal cases as the atlas for steroid withdrawal care (Color Atlas of Steroid Withdrawal from Topical Corticosteroid in Patients with Atopic Dermatitis, Ishiyaku Publishers, 2000). Below is the excerpt from this book.
----- Excerpt -----
Preface
I bet it is not easy to stop administering topical corticosteroids (TCS) to patients with atopic dermatitis (AD) for dermatologists who have not taken such measures.
This book visually describes the process of AD patients withdrawing from steroid addiction through recurrence of severe flare (rebound) with time-series color pictures.
There are some patterns in recurrence of AD flare (rebound flare) accompanying TCS withdrawal and the remission processes are classified into several types. This book was written to pass such information to dermatologists with littlie experience in the topical steroid withdrawal.
AD can be treated effectively with TCS for a short duration. But long time application is likely to cause severe recurrence of AD flare (rebound) after cessation.
I’d be happy if this book provides useful materials for dermatologists in objectively reviewing how to utilize TCS for AD treatment from the specialist’s viewpoint.
Type 1 Flush and plaque pattern
The lesion is characterized by poorly demarcated flushed plaques. In some severe cases, an entire body is flushed or erythroderma develops, but the cutaneous findings are simple and rarely present pigmentation, prurigo or lichenification.
When erythroderma develops, clearly demarcated flushed plaque frequently appears on the wrists or ankles.
This type is regarded as nearly pure atopic dermatitis because it is observed also in patients with no use of steroids for a long time after withdrawal and babies or infants with little use of steroids.
The flushed plaque may progress to exudative erythematous appearance in prolonged cases in which rebounds persist for months or over one year.
Because the TCS application period was not so long in the following case, it is probable that this clinical course is a natural healing process itself, which is common in infants or children, rather than the results of steroid withdrawal. After exudative erythematous appearance persists for months, eruption disappears.
Type 1 eruption is frequently seen as a recurrence long after withdrawal and often responds to disinfection, elimination of aggravating factors such as environmental antigens, food antigens and emotional stress and so on
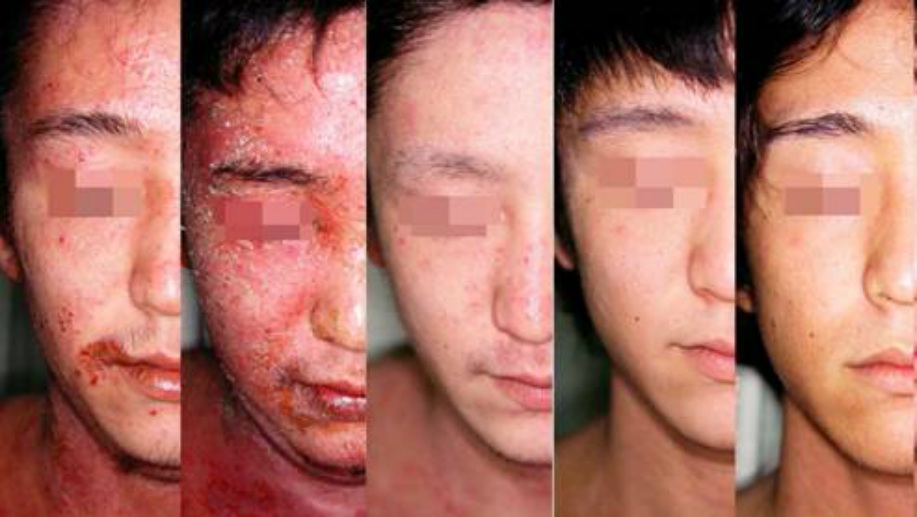
Type 2 Erythema fusing pattern
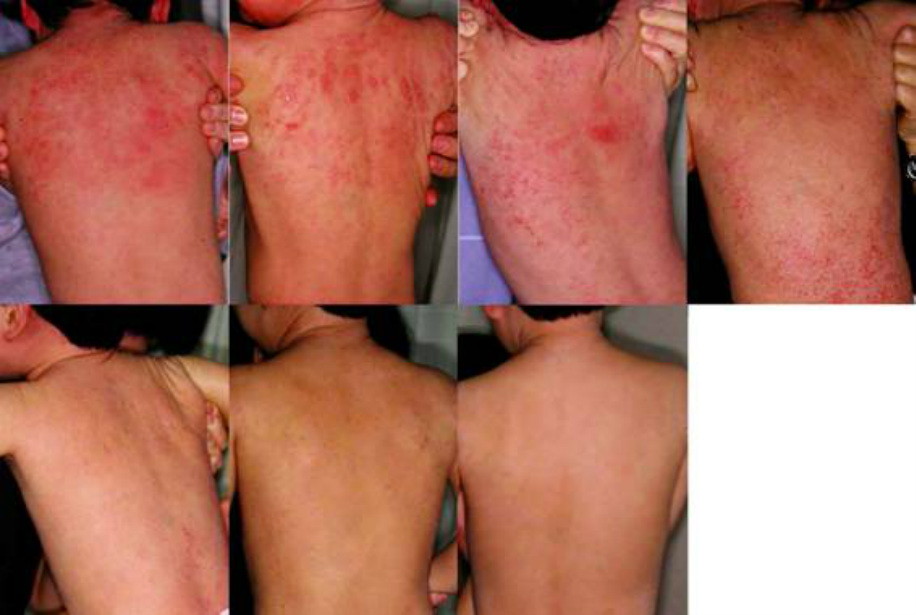
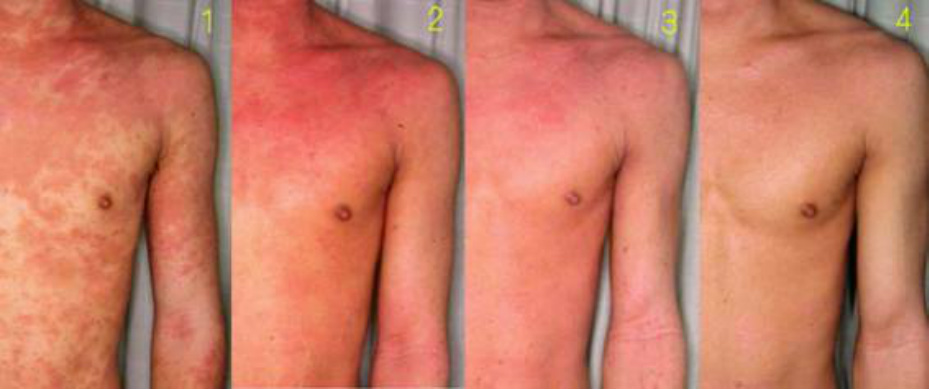
Small macular lesions with rather obvious demarcation spread to fuse to each other, which often develop into erythroderma and disappear. The lesion before the fusion may be either reddish (erythematous) or brownish. The reddish lesion resembles urticaria or measles and the brownish one resembles Type 3 eruption that will be mentioned as a geographically diffusing pattern in later part.
Type 2 is not the characteristic eruption immediately after the steroid withdrawal as Type 1 is not. Type 2 eruption can develop several months after the first aggravation following the withdrawal subsided. (The recurrence of flare long after the withdrawal is not as severe as the first one in most cases).
Type 2 Erythema fusing pattern
Small macular lesions with rather obvious demarcation spread to fuse to each other, which often develop into erythroderma and disappear. The lesion before the fusion may be either reddish (erythematous) or brownish. The reddish lesion resembles urticaria or measles and the brownish one resembles Type 3 eruption that will be mentioned as a geographically diffusing pattern in later part.
Type 2 is not the characteristic eruption immediately after the steroid withdrawal as Type 1 is not. Type 2 eruption can develop several months after the first aggravation following the withdrawal subsided. (The recurrence of flare long after the withdrawal is not as severe as the first one in most cases).
Type 2 eruption is not specific to the occasion of withdrawal but considered as a recurrence of atopic dermatitis itself.
However, it should be noted that the later aggravation is often less severe and resides faster than the previous one. That is, it is possible that the flare is amplified immediately after the withdrawal from steroids. In that sense, this type can be also included in steroid dermopathy.
The eruption usually starts on the face and, after the face symptom resides, moves to the chest or upper extremities.
In the case of developing erythroderma, the eruption moves to the wrists, dorsal hands and then lower extremities. Sometimes severe edema is observed in the lower extremities.
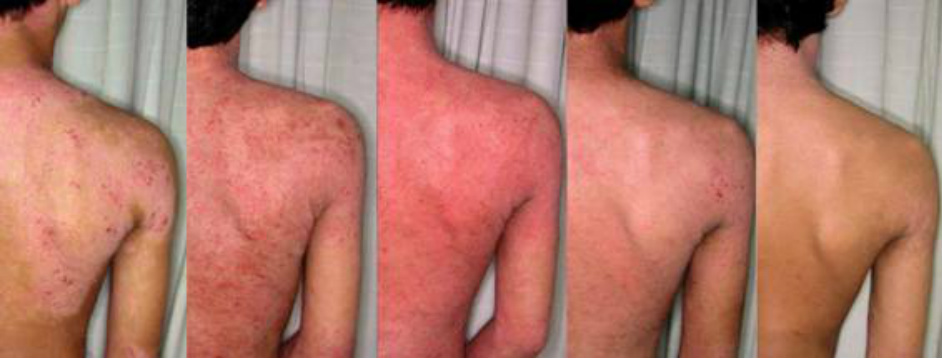
Type 3 Geographically diffusing pattern
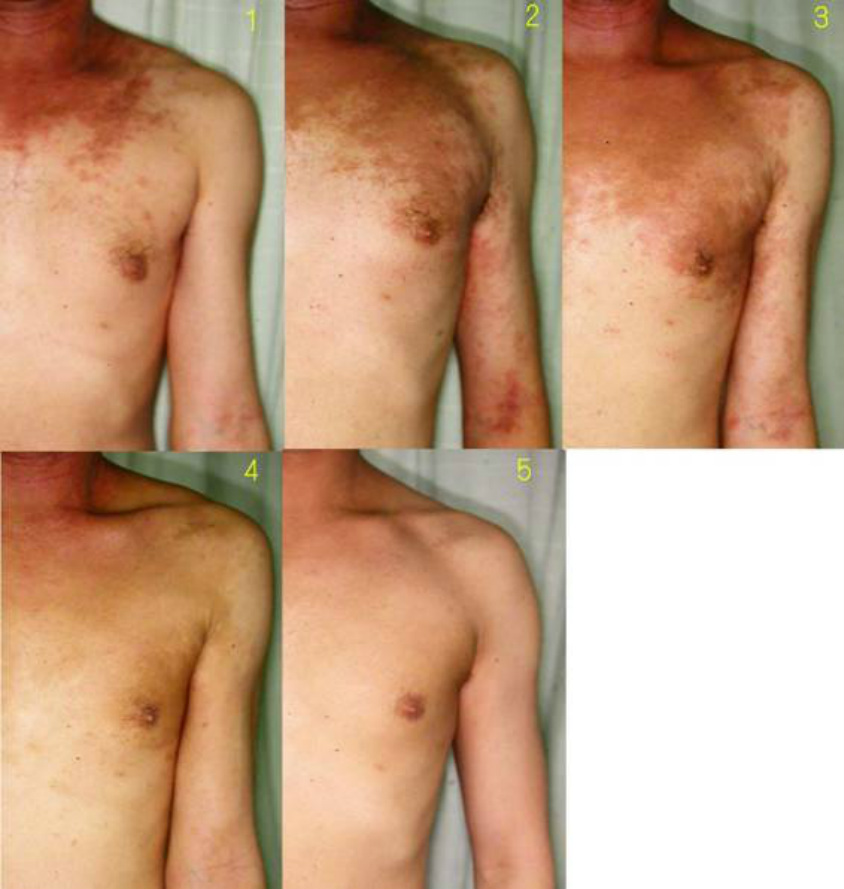
In this type, an irregular and rather large geographical eruption gradually expands and diminishes.
The eruption is a plaque with variegated reddish to brown color initially and becomes poorly demarcated as the diffusion progresses gradually. It vanishes after becoming a brown color predominant lesion or a brown pigmentation itself.
This type often responds to the disinfectant therapy. Erythroderma rarely develops. Sometimes severe eczema on hands accompanies.
However, it should be noted that the later aggravation is often less severe and resides faster than the previous one. That is, it is possible that the flare is amplified immediately after the withdrawal from steroids. In that sense, this type can be also included in steroid dermopathy.
The eruption usually starts on the face and, after the face symptom resides, moves to the chest or upper extremities.
In the case of developing erythroderma, the eruption moves to the wrists, dorsal hands and then lower extremities. Sometimes severe edema is observed in the lower extremities.
Type 3 Geographically diffusing pattern
In this type, an irregular and rather large geographical eruption gradually expands and diminishes.
The eruption is a plaque with variegated reddish to brown color initially and becomes poorly demarcated as the diffusion progresses gradually. It vanishes after becoming a brown color predominant lesion or a brown pigmentation itself.
This type often responds to the disinfectant therapy. Erythroderma rarely develops. Sometimes severe eczema on hands accompanies.
The brown lesion, which is irregular and geographical rather than macules expands and gradually diminishes. This type often arises at the neck and gradually expands and diminishes.
Typical type 3 lesion seldom recurs. In case of recurrence, a lesion is liable to develop as papules or more poorly demarcated mild erythema, which coincide with typical or classically described atopic dermatitis.
The dermatitis of type 3 is sometimes accompanied by severe eczema on hands expanding to the palm, the reason for which is not obvious though. It is a severe eczematous reaction with pustules and crusts and subsides in concurrence with or a little later than other symptoms.
Typical type 3 lesion seldom recurs. In case of recurrence, a lesion is liable to develop as papules or more poorly demarcated mild erythema, which coincide with typical or classically described atopic dermatitis.
The dermatitis of type 3 is sometimes accompanied by severe eczema on hands expanding to the palm, the reason for which is not obvious though. It is a severe eczematous reaction with pustules and crusts and subsides in concurrence with or a little later than other symptoms.
Type 4 Fulminant pattern
Severe and variegated eruption consisting of flushed plaque and other components such as exudates, crust, desquamation, pigmentation and excoriation develop between several weeks and one or two months after withdrawal. Rather rapid improvement is likely to follow between several weeks and months.
In most cases, papules or prurigos that are resistant to steroids are scattered before withdrawal. The difference between Type 4 and Type 5 (prurigo diffusing pattern) lies in that Type 4 has more furious eruption.
Sometimes fever exceeding 40°C continues for seven to ten days. In most cases, a temporary absence from school/work or hospitalization is necessary at the worst period.
In spite of thus severe systemic symptoms, the patients often reject suppressing them by temporal injection or resumption of steroids. Most patients seem to be aware that the condition is obviously caused by side effect of steroids from their own experiences.
Severe and variegated eruption consisting of flushed plaque and other components such as exudates, crust, desquamation, pigmentation and excoriation develop between several weeks and one or two months after withdrawal. Rather rapid improvement is likely to follow between several weeks and months.
In most cases, papules or prurigos that are resistant to steroids are scattered before withdrawal. The difference between Type 4 and Type 5 (prurigo diffusing pattern) lies in that Type 4 has more furious eruption.
Sometimes fever exceeding 40°C continues for seven to ten days. In most cases, a temporary absence from school/work or hospitalization is necessary at the worst period.
In spite of thus severe systemic symptoms, the patients often reject suppressing them by temporal injection or resumption of steroids. Most patients seem to be aware that the condition is obviously caused by side effect of steroids from their own experiences.
Type 5 Prurigo diffusing pattern
The prurigo scattered on the whole body that appears normal turns into erythroderma after withdrawal. Prurigo or prurigo-like nodes flattens and remains as excoriation for a while.
The progress is often persistent and long. It needs months or years till the rebound begins to subside. Much endurance is required of both the patient and therapist.
The type 5 pattern is a characteristic withdrawal dermatitis like Type 4 (fulminant pattern) and is different from a simple aggravation of atopic dermatitis.
The prurigo scattered on the whole body that appears normal turns into erythroderma after withdrawal. Prurigo or prurigo-like nodes flattens and remains as excoriation for a while.
The progress is often persistent and long. It needs months or years till the rebound begins to subside. Much endurance is required of both the patient and therapist.
The type 5 pattern is a characteristic withdrawal dermatitis like Type 4 (fulminant pattern) and is different from a simple aggravation of atopic dermatitis.
----- End of excerpt -----
In summary, Types 1 and 2 are not addictive or slightly addictive cases. Type 3 seems relevant to steroid resistance, and Types 4 and 5 are typical addictive cases. As mentioned above, sorting time-series progress into some patterns helps predict, to a certain extent, the withdrawal course that a patient may take.
I think such pattern recognition and classification are seldom chosen as study subjects in recent dermatology, for it cannot be quantified and it is difficult to be completed as a paper.
I myself regard the pattern recognition a spectacular art that dermatologists can be proud of. Reviewing the steroid withdrawal from this point of view is clinically and academically very interesting, isn’t it?
In summary, Types 1 and 2 are not addictive or slightly addictive cases. Type 3 seems relevant to steroid resistance, and Types 4 and 5 are typical addictive cases. As mentioned above, sorting time-series progress into some patterns helps predict, to a certain extent, the withdrawal course that a patient may take.
I think such pattern recognition and classification are seldom chosen as study subjects in recent dermatology, for it cannot be quantified and it is difficult to be completed as a paper.
I myself regard the pattern recognition a spectacular art that dermatologists can be proud of. Reviewing the steroid withdrawal from this point of view is clinically and academically very interesting, isn’t it?