Chapter 33 Approach to Multifactorial Disease
Residential Environment and Steroid Withdrawal in Atopic Dermatitis Treatment
By M Fukaya published in the Jpn. J. Allergol. 48(5) p.520-525 (1999)
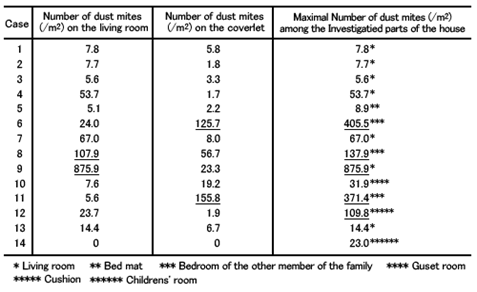
This is the paper I wrote in Japanese and submitted to the Japanese Journal of Allergology in 1999. This was the follow-up study of 14 patients whose residential environment had been investigated. Living conditions differ from person to person. The following table shows the mite density in the dust collected in each patient’s house.
Residential Environment and Steroid Withdrawal in Atopic Dermatitis Treatment
By M Fukaya published in the Jpn. J. Allergol. 48(5) p.520-525 (1999)
This is the paper I wrote in Japanese and submitted to the Japanese Journal of Allergology in 1999. This was the follow-up study of 14 patients whose residential environment had been investigated. Living conditions differ from person to person. The following table shows the mite density in the dust collected in each patient’s house.
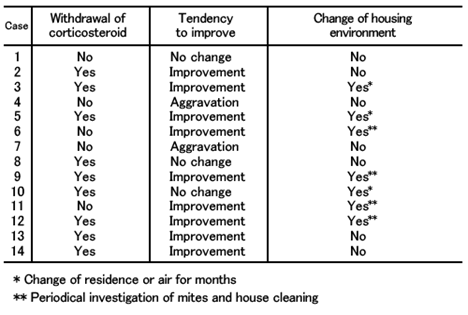
A survey was conducted 1 year later again to check if the living environment of patients had changed and classified into“Yes”when the house showed marked improvement in dust mite density or the living environment had changed due to changing the place of residence. Indicated below is the two-by-two contingency table between the environmental change and the AD conditions (aggravation or no change/improvement). According to Fisher’s exact probability test, p=0.143(>0.05)and there was no significant difference at a significance level of 5%.
In 14 patients, some were using corticosteroids and others were not. Therefore, I divided the patients into those who had refrained from steroid for a year (Yes) and those who had not (No) to check the AD conditions (aggravation or no change/improvement). In this case, p=0.266 and there was no significant difference too.
The breakdown of patients is as follows.
All patients do not refuse steroids. The case 1 patient was using steroids who had no change in residential environment and skin conditions.
Then, the test was performed with two groups that experienced either housing environmental changes or corticosteroid withdrawal (Yes) and that did neither (No). In this case, p=0.028 and there was significant difference at a significance level of 5%.
Then, the test was performed with two groups that experienced either housing environmental changes or corticosteroid withdrawal (Yes) and that did neither (No). In this case, p=0.028 and there was significant difference at a significance level of 5%.
I found these results very interesting. It is often said that AD is a multifactorial skin disorder. Some achieve remission through steroid withdrawal, while others recover by improving their dwelling environment. But there are people for whom neither is effective. In the follow-up study focusing on one factor, a statistically significant difference cannot be obtained when the sample size (n) is small. In such an occasion, testing across plural factors reveals significant difference. It is this approach we take in treating multifactorial diseases.
If we aim to gain the statistically significant difference as to a single factor, we may as well properly design the study and make the sample size much larger than the number of factors. But the purpose of clinical service is making patients recover from disorders (i.e. making efforts to make significant difference even if the sample size is small for the number of factors), and is not increasing the sample size until the significant difference can be gained as to a certain factor (this is the difference between the clinical service and the study).
I think it to be a clinical attitude in treating multifactorial diseases to repeat testing with other factors identified and added to see if the“p” value gets smaller as to 14 patients.
This was a basic stance I used to take when I treated AD patients. Though the theme of this book is topical steroid withdrawal, I did not always stick to the withdrawal as a dermatologist. Prolonged use of topical steroids is an important factor, but it is only one of the factors that make AD intractable disease.
Steroid withdrawal works in some cases. However there are other cases where it does not work and other means do well.
All patients who refrained from steroids in this study are not addicted to steroids. Case 6 patient, for example, was not using steroid, had a change in residential environment and improved in skin conditions. This patient was not addictive and the environment might have been the only factor that accelerated AD. As to the patients who had not used steroid (corticosteroid withdrawal) and achieved improvement 1 year later, what I observed might have been the process of recovery from rebound or the effect of environmental improvement which was prominent due to steroid discontinuation. (Definition of corticosteroid withdrawal when used in this paper.)
If we aim to gain the statistically significant difference as to a single factor, we may as well properly design the study and make the sample size much larger than the number of factors. But the purpose of clinical service is making patients recover from disorders (i.e. making efforts to make significant difference even if the sample size is small for the number of factors), and is not increasing the sample size until the significant difference can be gained as to a certain factor (this is the difference between the clinical service and the study).
I think it to be a clinical attitude in treating multifactorial diseases to repeat testing with other factors identified and added to see if the“p” value gets smaller as to 14 patients.
This was a basic stance I used to take when I treated AD patients. Though the theme of this book is topical steroid withdrawal, I did not always stick to the withdrawal as a dermatologist. Prolonged use of topical steroids is an important factor, but it is only one of the factors that make AD intractable disease.
Steroid withdrawal works in some cases. However there are other cases where it does not work and other means do well.
All patients who refrained from steroids in this study are not addicted to steroids. Case 6 patient, for example, was not using steroid, had a change in residential environment and improved in skin conditions. This patient was not addictive and the environment might have been the only factor that accelerated AD. As to the patients who had not used steroid (corticosteroid withdrawal) and achieved improvement 1 year later, what I observed might have been the process of recovery from rebound or the effect of environmental improvement which was prominent due to steroid discontinuation. (Definition of corticosteroid withdrawal when used in this paper.)