Chapter 26 Murine Model of Steroid addiction
Removal of the majority of epidermal Langerhans cells by topical or systemic steroid application enhances the effector phase pf murine contact hypersensitiveity.
By S Grabbe et al. published in the The Journal of Immunology, Vol. 155, Issue 9 4207-4217, 1995
This is the report on mice experiments conducted by German dermatologist, Dr. Grabbe. Dr. Cork said that prolonged use of Topical Corticosteroids causes epidermal barrier disruption via upregulated proteases and resulting barrier dysfunction allows antigen penetration, leading to flare rebound and steroid addiction. This theory currently recognized worldwide is consistent with Dr. Grabbe’s experiment results in 1995. There existed a person who gained test results supporting Dr. Cork’s theory 10 years earlier.
Dr. Grabbe concluded the Discussion as follows.
----- Excerpt -----
These data might also have clinical relevance, because they may help to explain the “rebound” phenomenon often seen in chronic eczema after steroid treatment, as well as the “angry back” syndrome seen in contact allergy patch tests after steroid treatment of the acute dermatitis. They may also offer a concept for understanding the prolonged duration of eczematous lesions after allergic skin reactions in chronically UV-exposed skin sites, such as in persistent light reaction or actinic reticuloid. Moreover, our data suggest that topical steroids may not be a first choice treatment in chronic eczematous diseases in which the Ag is unknown or cannot be avoided.
----- End of excerpt -----
His experiment began with sensitization of mouse ears using a chemical. Sensitization means making mice allergic to the chemical by causing a rash.
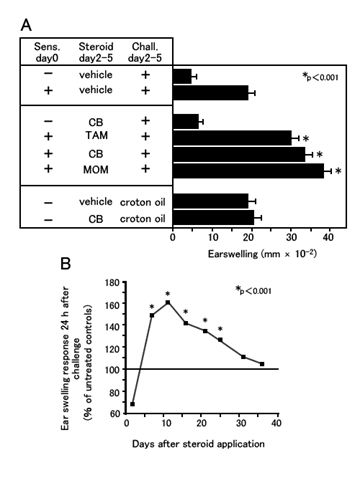
In “Sens. day 0” column of Figure A, “+” indicates topical application of the chemical and “-” indicates no application. CB, TAM, MOM are all topical steroids that were externally applied for 3 days from Day 2 to Day 5. In “Chall. day 16” column, “+” indicates chemical was applied again on Day 16 to monitor the response (ear swelling). If sensitization is established, ears should swell more on Day 16 than Day 0.
You can see the subjects treated with TCS for 3 days show more swelling than those only treated with the vehicle.
Removal of the majority of epidermal Langerhans cells by topical or systemic steroid application enhances the effector phase pf murine contact hypersensitiveity.
By S Grabbe et al. published in the The Journal of Immunology, Vol. 155, Issue 9 4207-4217, 1995
This is the report on mice experiments conducted by German dermatologist, Dr. Grabbe. Dr. Cork said that prolonged use of Topical Corticosteroids causes epidermal barrier disruption via upregulated proteases and resulting barrier dysfunction allows antigen penetration, leading to flare rebound and steroid addiction. This theory currently recognized worldwide is consistent with Dr. Grabbe’s experiment results in 1995. There existed a person who gained test results supporting Dr. Cork’s theory 10 years earlier.
Dr. Grabbe concluded the Discussion as follows.
----- Excerpt -----
These data might also have clinical relevance, because they may help to explain the “rebound” phenomenon often seen in chronic eczema after steroid treatment, as well as the “angry back” syndrome seen in contact allergy patch tests after steroid treatment of the acute dermatitis. They may also offer a concept for understanding the prolonged duration of eczematous lesions after allergic skin reactions in chronically UV-exposed skin sites, such as in persistent light reaction or actinic reticuloid. Moreover, our data suggest that topical steroids may not be a first choice treatment in chronic eczematous diseases in which the Ag is unknown or cannot be avoided.
----- End of excerpt -----
His experiment began with sensitization of mouse ears using a chemical. Sensitization means making mice allergic to the chemical by causing a rash.
In “Sens. day 0” column of Figure A, “+” indicates topical application of the chemical and “-” indicates no application. CB, TAM, MOM are all topical steroids that were externally applied for 3 days from Day 2 to Day 5. In “Chall. day 16” column, “+” indicates chemical was applied again on Day 16 to monitor the response (ear swelling). If sensitization is established, ears should swell more on Day 16 than Day 0.
You can see the subjects treated with TCS for 3 days show more swelling than those only treated with the vehicle.
Figure B shows the change in ear swelling according to the dates after TCS discontinuation. Swelling was the biggest on the 11th day and it took more than month to return to the original condition.
Dr. Grabbe initially assumed that topically applied steroid would suppress the later response, but he gained the opposite results. Dr. Grabbe had interest in this phenomenon and further confirmed that treating one ear with TPS increased the swelling of the treated ear, leaving the other ear unaffected, and that systemic application of steroids also increased the swelling.
As it was known that steroids, when topically used, reduced the number of Langerhans cells in the applicable skin, various investigations were conducted for Langerhans cells. Irradiating UVB (ultraviolet B), which also reduces Langerhans cells, increased the swelling in a dose-dependent manner. (Therefore he considered the experimental data might explain persistent light reaction or actinic reticuloid.) Topically applying steroids reduced Langerhans cells but did not totally remove Langerhans cells, and he took out the remaining cells to see the function and found that antigen-presenting function was preserved.
Dr. Grabbe postulated that: 1) Langerhans cells too young to be detected by marker or antigen presenting cells other than Langerhans might be functioning; 2) Macrophages migrating from the dermis might function as antigen presenting cells; and 3) Reduced Langerhans cells might facilitate the penetration of antigens, which will then directly act on other antigen presenting cells in the deeper layers such as dermis (e.g., macrophage) and cause a bigger response.
The third hypothesis seems to be consistent with Dr. Cork’s barrier disruption theory.
This experiment has been utilized as a steroid addiction-rebound model by many researchers and has helped to develop rebound-free or rebound-alleviating drugs.
Dr. Grabbe initially assumed that topically applied steroid would suppress the later response, but he gained the opposite results. Dr. Grabbe had interest in this phenomenon and further confirmed that treating one ear with TPS increased the swelling of the treated ear, leaving the other ear unaffected, and that systemic application of steroids also increased the swelling.
As it was known that steroids, when topically used, reduced the number of Langerhans cells in the applicable skin, various investigations were conducted for Langerhans cells. Irradiating UVB (ultraviolet B), which also reduces Langerhans cells, increased the swelling in a dose-dependent manner. (Therefore he considered the experimental data might explain persistent light reaction or actinic reticuloid.) Topically applying steroids reduced Langerhans cells but did not totally remove Langerhans cells, and he took out the remaining cells to see the function and found that antigen-presenting function was preserved.
Dr. Grabbe postulated that: 1) Langerhans cells too young to be detected by marker or antigen presenting cells other than Langerhans might be functioning; 2) Macrophages migrating from the dermis might function as antigen presenting cells; and 3) Reduced Langerhans cells might facilitate the penetration of antigens, which will then directly act on other antigen presenting cells in the deeper layers such as dermis (e.g., macrophage) and cause a bigger response.
The third hypothesis seems to be consistent with Dr. Cork’s barrier disruption theory.
This experiment has been utilized as a steroid addiction-rebound model by many researchers and has helped to develop rebound-free or rebound-alleviating drugs.